Lupron DEPOT-PED (leuprolide acetate for depot suspension) Injection, Powder, Lyophilized, For Suspension
Summary about Lupron DEPOT-PED
LUPRON DEPOT-PED is a gonadotropin-releasing hormone (GnRH) agonist. It’s a medicine that is similar to GnRH, a hormone made naturally by your body. LUPRON DEPOT-PED works by suppressing the natural GnRH hormone. This interrupts the release of the hormones that cause puberty until it is a more appropriate time for puberty to occur.
Since LUPRON DEPOT-PED works by interfering with the production of hormones that cause puberty, after the first month of treatment, your child’s signs of puberty should slow or stop. For girls, breast development will stop and may regress. For boys, the penis and testicles may shrink back to a size that is normal for their age.

After starting LUPRON DEPOT-PED therapy, your child may show increased signs and symptoms of CPP during the first few weeks of treatment. That’s normal, so don’t worry. It’s due to the way the medicine works. After the first few weeks, your child will stop making some hormones and you may see pubertal changes stop or slow down.
LUPRON DEPOT-PED 7.5 mg, 11.25 mg, and 15 mg for 1-month and 11.25 mg and 30 mg for 3-month administration are prescribed for the treatment of children with central precocious puberty (CPP).
During the first 2 to 4 weeks of treatment, LUPRON DEPOT-PED can cause an increase in some hormones. During this time, you may notice more signs of puberty in your child, including vaginal bleeding.
Some people taking gonadotropin-releasing hormone (GnRH) agonists like LUPRON DEPOT-PED have had new or worsened mental (psychiatric) problems. Mental (psychiatric) problems may include emotional symptoms such as:
– Crying
– Irritability
– Restlessness (impatience)
– Anger
– Acting aggressive
Lupron DEPOT-PED (leuprolide acetate for depot suspension) |
|
Active Ingredient |
leuprolide acetate |
Administration Route |
Intramuscular |
Alcohol Warning |
Both Lupron and alcohol can cause upset stomach, nausea, and dizziness.
Drinking alcohol while using Lupron may worsen these effects. Avoid or limit drinking alcohol while taking Lupron. |
Available Strength |
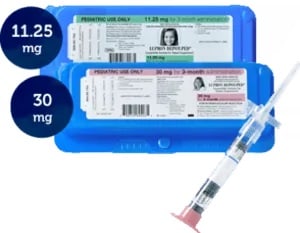
LUPRON DEPOT-PED 7.5 mg, 11.25 mg, or 15 mg for 1-month administration and LUPRON DEPOT-PED 11.25 mg or 30 mg for 3-month administration is provided in a prefilled dual chamber syringe for intramuscular injection. |
Breastfeeding Warning |
Not indicated for use in adult women.
Excreted into human milk: Unknown The effects in the nursing infant are unknown. |
Clinical Pharmacology |
Pharmacodynamics
Used in the palliative treatment of advanced prostate cancer. Leuprolide is a luteinizing hormone agonist that results in suppression of testicular or follicular steroidogenesis. Pharmacokinetics Absorption LUPRON DEPOT-PED 7.5 mg, 11.25 mg, or 15 mg for 1-month administration Following a single LUPRON DEPOT-PED 7.5 mg for 1-month administration to adult patients, mean peak leuprolide plasma concentration was almost 20 ng/mL at 4 hours and then declined to 0.36 ng/mL at 4 weeks. However, intact leuprolide and an inactive major metabolite could not be distinguished by the assay which was employed in the study. Nondetectable leuprolide plasma concentrations have been observed during chronic LUPRON DEPOT-PED 7.5 mg administration, but testosterone levels appear to be maintained at castrate levels. LUPRON DEPOT-PED 11.25 mg or 30 mg for 3-month administration Following a single LUPRON DEPOT-PED 11.25 mg or 30 mg for 3-month administration to children with CPP, leuprolide concentrations increased with increasing dose with mean peak leuprolide plasma concentration of 19.1 and 52.5 ng/mL at 1 hour for the 11.25 and 30 mg dose levels, respectively. The concentrations then declined to 0.08 and 0.25 ng/mL at 2 weeks after dosing for the 11.25 and 30 mg dose levels. Mean leuprolide plasma concentration remained constant from month 1 to month 3 for both 11.25 and 30 mg doses. The mean leuprolide concentrations 3 months after the first and second injections were similar indicating no accumulation of leuprolide from repeated administration. Distribution The mean steady-state volume of distribution of leuprolide following intravenous bolus administration to healthy male volunteers was 27 L. In vitro binding to human plasma proteins ranged from 43% to 49%. Metabolism In healthy male volunteers, a 1 mg bolus of leuprolide administered intravenously revealed that the mean systemic clearance was 7.6 L/h, with a terminal elimination half-life of approximately 3 hours based on a two compartment model. In rats and dogs, administration of 14C-labeled leuprolide was shown to be metabolized to smaller inactive peptides; a pentapeptide (Metabolite I), tripeptides (Metabolites II and III) and a dipeptide (Metabolite IV). These fragments may be further catabolized. The major metabolite (M-I) plasma concentrations measured in 5 prostate cancer patients reached maximum concentration 2 to 6 hours after dosing and were approximately 6% of the peak parent drug concentration. One week after dosing, mean plasma M-I concentrations were approximately 20% of mean leuprolide concentrations. Excretion Following administration of LUPRON DEPOT 3.75 mg to 3 patients, less than 5% of the dose was recovered as parent and M-I metabolite in the urine. Specific Populations The pharmacokinetics of LUPRON DEPOT-PED has not been determined in patients with hepatic or renal impairment. |
Cost |
Approximate Retail Price according to https://www.drugs.com/price-guide/lupron-depot-ped
Intramuscular kit: · 7.5 mg/month: $1,641.68 · 11.25 mg/3 months: $8,903.59 Intramuscular Powder For Injection, Extended Release: · 11.25 mg/month: $2,973.52 · 15mg/month: $3,274.18 · 30mg/3 months: $9,805.54 |
Dosage Form |
Injection, powder lyophilized for suspension |
Dose Schedule |
Dose and Principles of Dosing 7.5 mg, 11.25 mg, or 15 mg for 1-month administration
LUPRON DEPOT-PED must be administered under the supervision of a physician. LUPRON DEPOT-PED is administered as a single intramuscular injection once a month. The starting dose will be dictated by the child’s weight, as indicated in the table below. The dose of LUPRON DEPOT-PED must be individualized for each child. If adequate hormonal and clinical suppression is not achieved with the starting dose, it should be increased to the next available higher dose (e.g. 11.25 mg or 15 mg at the next monthly injection). Similarly, the dose may be adjusted with changes in body weight. The injection site should be varied periodically. The goal of therapy is to suppress pituitary gonadotropins and peripheral sex steroids, and to arrest progression of secondary sexual characteristics. Hormonal and clinical parameters should be monitored after 1–2 months of initiating therapy and with each dose change to ensure adequate pituitary gonadotropin suppression. Once a dose that results in adequate hormonal suppression is found, it can often be maintained for the duration of therapy in most children. It is recommended, however, that adequate hormonal suppression be verified in such patients as weight can increase significantly while on therapy. Each LUPRON DEPOT-PED strength and formulation has different release characteristics. Do not use partial syringes or a combination of syringes to achieve a particular dose. LUPRON DEPOT-PED should be discontinued at the appropriate age of onset of puberty at the discretion of the physician. Dose and Principles of Dosing 11.25 mg or 30 mg for 3-month administration LUPRON DEPOT-PED 11.25 mg or 30 mg for 3-month administration must be administered under the supervision of a physician. LUPRON DEPOT-PED 11.25 mg or 30 mg for 3-month administration should be administered once every three months (12 weeks) as a single intramuscular injection. Regardless of the dose chosen, the goal of therapy is to suppress pituitary gonadotropins and peripheral sex steroids, and to arrest progression of secondary sexual characteristics. Hormonal and clinical parameters should be monitored during treatment, for instance at month 2-3, month 6 and further as judged clinically appropriate, to ensure adequate suppression. In case of inadequate suppression, other available GnRH agonists indicated for the treatment of CPP should be considered. Each LUPRON DEPOT-PED 11.25 mg or 30 mg for 3-month administration strength and formulation has different release characteristics. Do not use partial syringes or a combination of syringes to achieve a particular dose. LUPRON DEPOT-PED 11.25 mg or 30 mg for 3-month administration treatment should be discontinued at the appropriate age of onset of puberty at the discretion of the physician. |
Drug Class |
L02AE – Gonadotropin releasing hormone analogues |
Drug Unit |
mg |
Food Warning |
No known interactions |
Included In
|
Eligibility: Available to patients with commercial prescription insurance coverage for LUPRON DEPOT-PED who meet eligibility criteria. Co-pay assistance program is not available to patients receiving prescription reimbursement under any federal, state or government-funded insurance programs (for example, Medicare (including Part D), Medicare Advantage, Medigap, Medicaid, TRICARE, Department of Defense or Veteran’s Affairs programs) or where prohibited by law or by the patient’s health insurance provider. If at any time the patient begins receiving prescription drug coverage under any such federal, state or government-funded healthcare program, patient will no longer be able to use the LUPRON DEPOT-PED Instant Savings Card and patient must call 1-877-832-9755 to stop participation. Patients residing in or receiving treatment in certain states may not be eligible. Patients may not seek reimbursement for value received from the Instant Savings Card from any third-party payers. Offer subject to change or discontinuance without notice. Restrictions, including monthly maximums, may apply. |
Interacting Drugs |
No pharmacokinetic-based drug-drug interaction studies have been conducted; however, drug interactions are not expected to occur.
Drug/Laboratory Test Interactions:
|
Is Available Generically |
No. There is currently no therapeutically equivalent version of Lupron Depot-PED available. |
Is Proprietary |
Yes |
Label Details |
https://www.accessdata.fda.gov/drugsatfda_docs/label/2011/020263s036lbl.pdf |
Legal Status |
Legal.
Is not subject to the Controlled Substances Act. |
Manufacturer |
AbbVie Inc. |
Maximum Intake |
15 mg in one dose for 1-month; 30mg in one dose for 3 months.
LUPRON DEPOT-PED must be administered under the supervision of a physician. |
Mechanism of Action |
Leuprolide acetate, a GnRH agonist, acts as a potent inhibitor of gonadotropin secretion when given continuously and in therapeutic doses. Human studies indicate that following an initial stimulation of gonadotropins, chronic stimulation with leuprolide acetate results in suppression or “downregulation” of these hormones and consequent suppression of ovarian and testicular steroidogenesis. These effects are reversible on discontinuation of drug therapy.
Leuprolide acetate is not active when given orally. |
Non Proprietary Name |
Leuprolide acetate |
Overdosage |
In early clinical trials using leuprolide acetate in adult patients, doses as high as 20 mg/day for up to two years caused no adverse effects differing from those observed with the 1 mg/day dose.
In rats, subcutaneous administration of leuprolide acetate as a single dose 225 times the recommended human pediatric dose, expressed on a per body weight basis, resulted in dyspnea, decreased activity, and local irritation at the injection site. There is no evidence at present that there is a clinical counterpart of this phenomenon. In cases of overdosage, standard of care monitoring and management principles should be followed. |
Pregnancy Category |
AU TGA pregnancy category D: Drugs which have caused, are suspected to have caused or may be expected to cause, an increased incidence of human fetal malformations or irreversible damage. These drugs may also have adverse pharmacological effects. Accompanying texts should be consulted for further details.US FDA pregnancy category X: Studies in animals or humans have demonstrated fetal abnormalities and/or there is positive evidence of human fetal risk based on adverse reaction data from investigational or marketing experience, and the risks involved in use of the drug in pregnant women clearly outweigh potential benefits. |
Pregnancy Warning |
-If a patient becomes pregnant during treatment, use should be discontinued. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to the fetus.
-Patients should be advised that if they miss any doses, breakthrough bleeding or ovulation may occur with the potential for conception. Animal studies have shown reproductive toxicity. Additionally, there was increased fetal mortality and decreased fetal weights in animals. There are no controlled data in human pregnancy. |
Prescribing Info |
https://www.accessdata.fda.gov/drugsatfda_docs/label/2011/020263s036lbl.pdf |
Prescription Status |
Prescription drug |
Proprietary Name |
Lupron DEPOT-PED |
Related Drugs |
Bicalutamide, Leuprolide, Triptorelin, Goserelin, Buserelin |
RxCUI |
1433514 203852 |
Warning |
Initial Rise of Gonadotropins and Sex Steroid LevelsDuring the early phase of therapy, gonadotropins and sex steroids rise above baseline because of the initial stimulatory effect of the drug. Therefore, an increase in clinical signs and symptoms of puberty may be observed.Psychiatric EventsPsychiatric events have been reported in patients taking GnRH agonists, including LUPRON DEPOT-PED. Postmarking reports with this class of drugs include symptoms of emotional lability, such as crying, irritability, impatience, anger and aggression. Monitor for development or worsening of psychiatric symptoms during treatment with LUPRON DEPOT-PED.ConvulsionsPostmarketing reports of convulsions have been observed in patients receiving GnRH agonists, including leuprolide acetate. These included patients with a history of seizures, epilepsy, cerebrovascular disorders, central nervous system anomalies or tumors, and patients on concomitant medications that have been associated with convulsions such as bupropion and SSRIs. Convulsions have also been reported in patients in the absence of any of the conditions mentioned above.Monitoring and Laboratory TestsResponse to LUPRON DEPOT-PED 7.5 mg, 11.25 mg, or 15 mg for 1-month administration should be monitored with a GnRHa stimulation test, basal LH or serum concentration of sex steroid levels beginning 1-2 months following initiation of therapy, with changing doses, or potentially during therapy in order to confirm maintenance of efficacy. Measurement of bone age for advancement should be done every 6-12 months.Response to LUPRON DEPOT-PED 11.25 mg or 30 mg for 3-month administration should be monitored with a GnRHa stimulation test, basal LH or serum concentration of sex steroid levels at months 2-3, month 6 and further as judged clinically appropriate, to ensure adequate suppression. Additionally, height (for calculation of growth rate) and bone age should be assessed every 6-12 months.Once a therapeutic dose has been established, gonadotropin and sex steroid levels will decline to prepubertal levels. Gonadotropins and/or sex steroids may increase or rise above prepubertal levels if the dose is inadequate. Noncompliance with drug regimen or inadequate dosing may result in inadequate control of the pubertal process with gonadotropins and/or sex steroids increasing above prepubertal levels. |
Links:
https://www.lupronped.com/
https://www.drugs.com/cdi/lupron-depot-ped.html
https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=e99f47d2-da10-3127-ecb3-e5d942ae6e81
https://www.drugbank.ca/drugs/DB00007